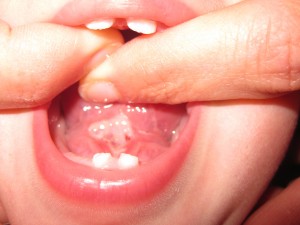
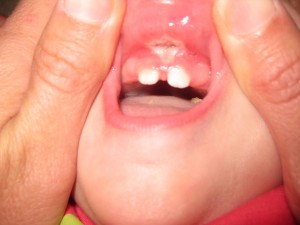
Pain, Bleeding and Appearance
The discomfort from lip and tongue-tie release usually only lasts for about 24 hrs, although in older babies/toddlers the discomfort may last about 48 hrs. If a lip-tie was released, you may notice some swelling of the lip for a few days after the procedure. Breastfeeding and skin-to-skin contact provide natural pain relief, however your baby may need something for pain if they are really fussy or refusing to feed in the first 24-48 hrs. Acetaminophen (Tylenol/Tempra), and homeopathics are both effective forms of pain relief. What you give is a personal decision based on what you are most comfortable with. If you are giving medication, please check with your doctor or pharmacist for the appropriate dose and to make sure that the medication is right for your child. Remember that dosages should be based on a child’s weight, not age. Children under the age of 2 months should not be given ibuprofen (Motrin/Advil) and children should never be given aspirin due to the risk of Reye’s syndrome. Topical numbing ointments containing benzocaine (ex. Orajel/Anbesol) should not be used due to health risks (FDA).
There is usually very little bleeding with tongue and lip-tie release, especially if a laser is used. If your child experiences any bleeding after the procedure, direct pressure on the area should quickly stop it. If bleeding seems excessive or you are concerned, then please contact your doctor or whoever did the procedure.
If your baby swallowed any blood during the procedure, you may notice some blood in your child’s diaper or spit-up in the first 24hrs after the procedure. If it continues beyond 24 hrs, is excessive or you are concerned, then please contact your doctor.
The areas where the ties were released will be white or yellowish in appearance, This is normal healing and is not an indication of infection. Full healing takes a few weeks.
Stretching Exercises
Research on the need for stretching exercises is limited, however the experiences of many of us in the profession suggest that stretching exercises after lip and tongue-tie release help to reduce the risk of reattachment and the need for further procedures.
Before starting the stretching exercises, make sure that your hands are clean and your nails are short to avoid accidentally hurting your baby. To stretch the lip. you want to pull the lip out and up towards your baby’s nose, applying gentle pressure to expose the area where the release was made (see picture above). For the tongue, most parents find it easiest to position baby on their back with their head towards you and feet pointing away from you. Use your index fingers to get under your baby’s tongue and elevate it so that the area where the release was made is exposed (see picture above). After holding the stretch for 3-5 seconds, position your fingers on either side of the diamond shape where the release was made, and pull your finger apart for 3-5 seconds to stretch the surgical site horizontally.
I recommend starting the stretching exercises at the second feeding after the procedure, and stretching 6 times in 24 hours, including at least one stretching session overnight. Stretches should be quick, you only need to hold them for 3-5 seconds. After the first 24 hours, you can add in gentle massage of the surgical sites, done for a few seconds after you do the stretches. Stretching should be continued for at least 7-10 days after the procedure. For some babies healing may take a little longer, so if you stop the stretches and breastfeeding becomes uncomfortable again, then start the exercises again and continue for another week. (C. Watson Genna, personal communication, June 17, 2011)
Video of stretching and massage from Dr. Kotlow
When you do the exercises depends on what works best for you and your baby. Some babies do well with doing the exercises just before feeding because nursing helps them to calm down. Some babies seem to become a little disorganized after stretches and don’t nurse as well, so for these babies, doing the stretches in between feedings, for example during diaper changes, tends to work best.
Babies usually don’t like the stretches, and they may cry or fuss but they should calm down quickly once you are done. Many moms find that a few drops of Rescue Remedy given 10-15 minutes before doing the stretches can help make the stretches easier. Along with doing the stretches, it is a good idea to provide lots of opportunities for positive stimulation around your baby’s mouth. Lots of kisses, stroking and gentle massage can help to minimize any negative associations from the procedure and stretching.
Handout: Care of Your Child After Tongue-Tie or Lip-Tie Release
Changes in sucking patterns
One of the most important things to understand when your child has a tongue and/or lip-tie released is that improvement is rarely immediate. The release of the frenulum is usually just the first step. Your baby will need some time to figure out what to do with the new mobility of their tongue.
The tongue is a muscle, and it becomes used to functioning in a certain way just like any other muscle in the body. When tongue function is restricted by a tongue-tie, the body adapts. Since the tongue isn’t able to function the way it’s supposed to, other muscles have to help compensate. In turn, the muscles that are compensating for the restricted tongue function now aren’t doing their job properly, so more muscles have to help compensate. You have one muscle that isn’t able to do it’s job properly, and it can lead to whole cascade of compensations and adaptations throughout the body. When a tongue-tie is released, the child has no muscle memory of how to use their tongue without the restriction there. It takes time for the brain to rewire itself and figure out how to suck effectively once the tie is released.
Bodywork
Many moms find that gentle bodywork such as chiropractic, craniosacral therapy, osteopathy, bowen therapy etc is an important part of the process of treating tongue and lip-tie. I’ve heard from numerous moms who saw some improvement after ties were released but didn’t see big improvement until after a few sessions of bodywork. The type of bodywork matters less than the skill of the practitioner. It’s important to find someone who is qualified and experienced at working with babies. The bodywork helps the child’s body release the adaptations that have formed while sucking with restricted tongue function, and it helps to speed up the process of the child figuring out how to suck effectively.
A note about bodywork: Sometimes, when bodywork is done after tongue-tie release, it can release other soft tissue restrictions which allows more frenulum to come forward. This frenulum may or may not need to be released, depending on how much it impacts the function of the tongue. This is not a case of reattachment, but rather a case of more frenulum becoming visible as other restrictions are released. For this reason, it is often beneficial to have some bodywork done before, as well as after tongue-tie release (if possible) to increase the chances of all of the frenulum being released with the first procedure.
If there is no one in your area who can perform bodywork on young children, or if it is not something you can afford, it certainly doesn’t mean that breastfeeding is doomed. Many moms see improvement in breastfeeding even without any bodywork (although bodywork can certainly speed up the process). Infant massage can also be beneficial and is something that you can do yourself for your baby. Gentle massage of your baby’s face, jaw and neck can help to loosen tense muscles and it’s a fun way to bond with your baby.
What to expect with nursing
As mentioned above, it is very normal to not notice much difference in nursing to start with. Sometimes there may even be a little bit of regression in sucking (things get worse instead of better) for a day or two as your child’s brain tries to sort out how to use their tongue now that the restriction is gone. Many moms report that they have a few good feedings and a lot of bad feedings in the early days. From what I have seen when watching babies nurse after tongue-tie release, it seems that fatigue can be an issue in the early days. It makes sense that when a muscle is being used in a way that it is not used too, it is going to get tired in the beginning until it strengthens (after my son’s tongue-tie was released, whenever he stuck his tongue out as far as he could – much farther than before the release – he would grab the back of neck and say “ow”. His muscles weren’t used to being used that way!).
Many moms find that some feedings go OK, and then feedings get worse as the day progresses. Gradually, as the tongue and other accessory muscles strengthen and get used to new patterns of use, there are more and more “good” feedings, until eventually all of the child’s nursing sessions are going well and the child is nursing effectively without causing mom any pain. In my experience with my clients, this process usually takes at least a week, sometimes longer. If you have been pumping and/or supplementing prior to the release of your child’s tongue and/or lip-tie, any changes to your routine should be made very gradually as you keep an eye on your baby’s weight gain.
Breastfeeding is the best form of sucking exercise after tongue-tie release and in babies under the age of 3 months, sucking issues tend to resolve spontaneously with practice at breast (C. Watson Genna, personal communication, June 17, 2011). If you are not seeing any improvement after 5-7 days, it’s a good idea to check with an International Board Certified Lactation Consultant (IBCLC) for further assistance (it’s also a good idea to consider bodywork for your child if you haven’t already). Sometimes it is necessary to introduce other sucking exercises but these should be tailored to the child’s specific needs by someone knowledgeable about breastfeeding.
References:
Hazelbaker, A. K. (2010). Tongue-tie: Morphogenesis, impact, assessment and treatment. Columbus, OH: Aidan and Éva Press.
Watson Genna, C. (2008). Supporting sucking skills in breastfeeding infants. Sudbury, MA.: Jones and Bartlett.
Tongue-tie and Lip-tie Resources
Please note that the information presented here is for educational purposes only and is not intended as medical advice. Please be sure to discuss your situation and treatment options with your own health care provider(s) in order to receive medical care that is suited to your and your child’s individual needs.